| In the first months of the pandemic, we got conflicting messages. Typically, the public was told that it was transmitted by large droplets, and protection meant staying 2 meters away from others, washing hands (and surfaces) frequently, and staying behind plexiglass barriers. On the other hand, healthcare workers were demanding N95 masks, which are certified for filtration of 0.3 micron particles!
Aerosol scientists were pointing out that aerosol transmission had been important in past respiratory disease epidemics, so there was no reason to expect otherwise from SARS-CoV2. Part of the confusion arises from inconsistent use of the terms “aerosol” and “droplet”. To an aerosol researcher (like me), an aerosol particle is a liquid or solid particle that is transported mainly by the motion of the surrounding gas – and this could include droplets up to 30 microns depending on circumstances. In the public health community, the dividing line between droplets and aerosols is set at either 3 or 5 microns. Thus, if transmission of COVID results from particles between 3 and 30 microns, reasonable people could refer to this as aerosol transmission or droplet transmission. Behind the confusion caused by terminology, there is a real question critical to what we do to control the spread of the virus. I’ve tried below to synthesize the issues, filling in gaps in the literature with “educated guesses”. Current masking policies are consistent with protection against a very wide range of particle sizes, and they also reduce emissions from an infected person. It is less clear, however, which engineering controls are helpful. If particles of concern are larger than 8-10 microns, improving the building ventilation system will have a very modest benefit, and could in fact create drafts that spread larger droplets – apparently an important factor in several restaurant case studies, where the zone of infected people was non-uniform in the room and roughly consistent with major air currents. Particles 10-30 microns are well into the “droplet” regime, but are still small enough to be carried across most rooms (and around those plexiglass barriers) by air currents before they settle to the ground. |
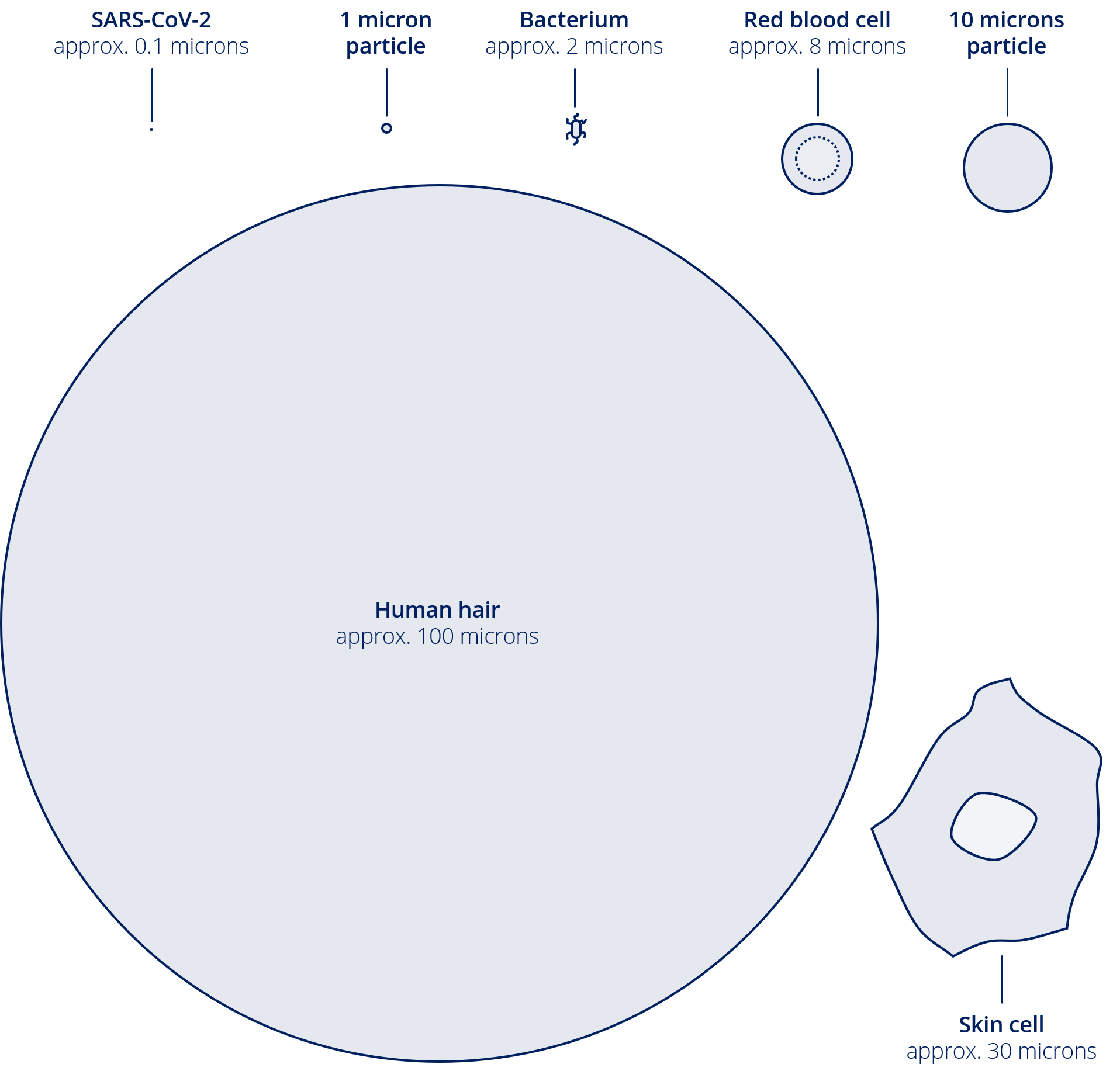
figure courtesy T. Sipkens |
| Particle Diameter
[microns] |
Primary PPE | Engineering controls | Transmission characteristics |
| 0.1 – 2 | N95 respirator, Level II surgical mask, powered air purifying respirator | Building ventilation with MERV 14 filters, HEPA filters, UV sterilization | Indoor exposure over many hours, spatially uniform, multi rooms |
| 2-8 | Well-fitted mask with decent filtration efficiency | Building ventilation, MERV 12-13 | Transmission uniform within rooms; exposure ~hour? |
| 8-15 | Any mask as long as it fits well | Local air extraction/filtration | Transmission <hour, non-uniform within room |
| 15-30 | Any mask if it fits; possibly some protection from face shields | Important to avoid strong drafts from fans and HVAC | Transmission follows air pathway in room; exposure of minutes; close range outdoor contact starts to become a risk |
| 30- 100 | Face shields and distance | Avoid strong drafts and install partitions | Transmission with a few meters of subject or direct air current; exposure of <min. Indoor or outdoor transmission probably equally likely |
| > 100 | Face shields and distance | Barriers and physical distancing | Indoor or outdoor transmission with very brief contacts within 2 meters |